Protein: Fake news
Despite the UK dietary guidelines recommending a healthy balanced diet,1 high protein diets are frequently perceived as the healthiest option.2 However, all macronutrients play an important role in the diet at every stage of life. As healthcare professionals, it can be difficult to navigate the fake news surrounding nutrition. How would you explain to a parent that a high protein diet is not necessarily a good thing for their baby? So what are the protein requirements of infants?
The first 1000 days
Stage of life is an important determinant of dietary requirements.3 Studies link excessive protein during the first 1000 days with increased infant weight gain and obesity later in life.4
Why protein?
Excessive protein intake in babies is a likely cause of accelerated growth in formula-fed infants due to insulinogenic amino acids,5–7 which stimulate the release of insulin, resulting in fat deposition.5–6

Breastfeeding is the optimal way to feed a baby8,9
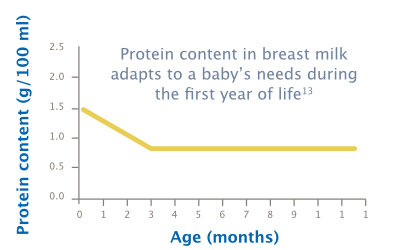
Breastfed babies tend to grow more slowly than formula-fed babies. This slower growth rate has shown significant long-term health benefits, including a lower risk of obesity and cardiovascular disease.8–12 The protein content of breast milk adapts to the infant’s requirements and decreases over the course of lactation in order to support age-appropriate growth.13,14
Protein in infant formula
Based on the latest science, some companies have lowered the protein in infant formula and follow-on formulae in recent years. The aim is to achieve a slower growth rate in formula-fed infants, comparable to that of a breastfed infant,15 and to help reduce the infant’s risk of becoming overweight or obese later in life.5
Feeding recommendations to protect against obesity include:
- Exclusive breastfeeding for the first 6 months of life with the introduction of appropriate complementary foods at 6 months alongside continued breastfeeding8
- If formula is being used, the use of a lower protein infant formula that has been clinically tested can support appropriate growth comparable to a breastfed baby15

Download the article

